What is Folliculitis ?
It is a condition caused due to infection of the hair follicles by Staphylococcus aureus or other bacteria. Some variants of folliculitis are also called barber’s itch or hot tub folliculitis. Extreme cases can result in scarring and permanent loss of hair. Mild cases of folliculitis can cause embarrassment and discomfort
The infection normally occurs as tiny pimples with white heads around hair follicles. A majority of cases are shallow and itchy, but occasionally can be painful. Shallow folliculitis tends to clear on its own within a few days, but recurrent and deep folliculitis may need medical care.
Symptoms of folliculitis
Some of the signs and symptoms of folliculitis are as follows:
- Scalp folliculitis affects the scalp hair follicles. It is also known as ‘Proprionibacterium folliculitis’ or ‘acne necrotica miliaris.’ It causes tiny, intensely itchy pustules within the scalp, primarily affecting the frontal hairline. The lesions may occur in small numbers or may be appear as many lesions. They tend to become sore and crust over.
- Superficial or shallow folliculitis which affects the top layer of the hair follicles can cause:
- Groups of tiny, pus filled or reddish lumps that forms around hair follicles
- Inflamed and reddened skin
- Pus filled blisters that rupture and experience crusting
- Tenderness or itchiness
- Deep folliculitis affects the complete hair follicle and begins deeper in the surrounding skin, causing:
- A big swollen lump or growth
- Pain
- Pus filled blisters that rupture and crust over
- Possible scarring after clearance of infection
Types of folliculitis
The superficial types of folliculitis are listed below:
- Staphylococcal folliculitis: It results in whitish, itchy, pus-filled lumps that can affect any area of the body containing hair follicles. When the condition occurs in a man’s beard region, then it is known as barber’s itch. It is caused due to infection of the hair follicle by staph bacteria. It may be noted that staph bacteria are normally present in all individuals, but usually lead to health problems when they enter the body via a wound or a cut. This can happen while shaving, scratching or skin trauma or injury.
- Pseudofolliculitis barbae: It refers to inflammation of the beard area hair follicles, and affects men due to the curving back of saved hairs into the skin. It causes inflammation and occasionally results in dark, elevated scars on the neck and face.
- Hot tub folliculitis: Also called pseudomonas folliculitis, it is caused due to infection by the pseudomonas bacteria which can flourish in different environments, which include hot tubs with unregulated levels of pH and chlorine. A rash comprising of circular, reddish, itchy bumps develops within 8 hours to 5 days post exposure to the bacteria, which may later form into tiny, pus-filled blisters.
- Pityrosporum folliculitis: It is caused due to yeast infection and results in reddish, itchy and persistent pustules on the chest and back and occasionally on the shoulders, neck, face and upper arms. It is more common in adult men and teenagers
The deep types of folliculitis are listed below:
- Sycosis barbae: It affects men who have started shaving and features inflammation of the entire hair follicle area. Initially, tiny pustules occur on the chin, upper lip, and jaw and later become more prominent due to continued shaving. Severe cases may lead to scarring.
- Boils and carbuncles: Deep infection of the hair follicles by staph bacteria results in sudden appearance of a pinkish or reddish, painful lump. There may also be redness and swelling of the surrounding skin. The lump later fills with pus and becomes more painful and bigger, before finally bursting and draining. Tiny boils normally heal without scaring, while large boils can cause scarring. A carbuncle refers to a cluster of boils affecting the shoulders, back of neck or back of thighs. It leads to a more severe and deeper infection as compared to single boils and hence experience slower formation and healing.
- Gram-negative folliculitis: It may result from prolonged antibiotic treatment which can affect the normal balance of bacteria living in the nose leading to excess growth of harmful pathogens, i.e. gram-negative bacteria. Stopping antibiotic therapy resolves the problem in most patients. However, in some affected people, it can result in new, intense acne lesions
- Eosinophilic folliculitis: It most affects HIV infected patients and causes recurrent blotches of pus-filled, inflamed sores on the face, upper arms or back. The condition tends to be extremely itchy, spreads and causes dark pigmentation of the affected skin.
Causes of folliculitis
- Folliculitis is caused due to hair follicle infection by bacteria, fungi or viruses, with the primary cause being staph infection. The condition is densest on the scalp but can affect all parts of the body, with the exceptions being the mucus membranes, soles and palms.
- Damage of the hair follicles due to shaving, perspiration, skin injuries inflammatory skin disorders, tight clothing, etc. can increase the susceptibility to developing folliculitis.
Treatment of folliculitis
- Staphylococcal folliculitis is treated with oral or topical antibiotics. Avoid shaving or shave with an electric razor or a new blade, till the infection heals
- Pseudofolliculitis barbae is treated by engaging in proper self-care and proper shaving procedures, use of shaving gels, moisturizers, etc.
- Pseudomonas folliculitis: The condition is treated as per individual cases, along with topical or oral medicines to alleviate itching. Severe cases may need oral antibiotic therapy
- Pityrosporum folliculitis is treated with oral and topical anti-fungal medications. Recurrent cases may require indefinite use of topical antifungal drugs.
- Gram-negative folliculitis may be caused due to prolonged use of antibiotics to cure acne, but this type of folliculitis is treated with topical or oral antibiotics
- Sycosis barbae: A topical antibiotic along with warm saline compresses may be suggested. Serious cases may require oral antibiotics
- Eosinophilic folliculitis: It is usually treated with topical corticosteroids, with severe cases requiring a short dosage of oral corticosteroids. HIV/AIDS patients with mild eosinophilic folliculitis may be treated with oral antihistamines along with topical steroids.
- Doctors may treat boils and carbuncles by draining the skin abnormalities via an incision. Recurrent and severe cases may need treatment with antibiotics.
Folliculitis Pictures
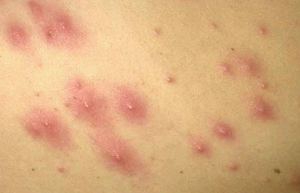
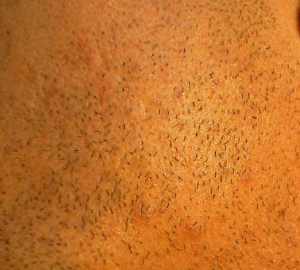
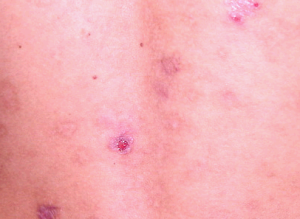
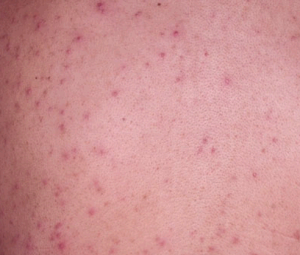
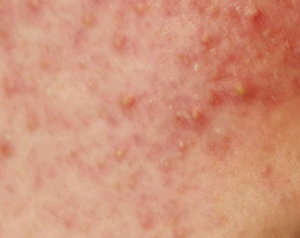
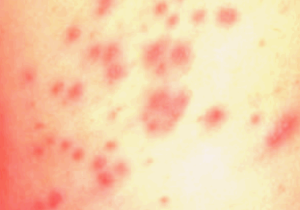
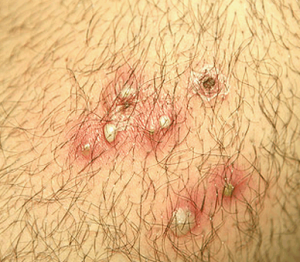
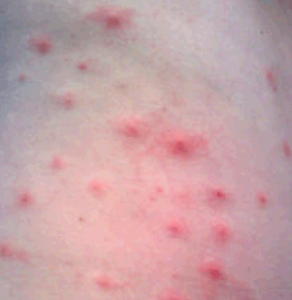
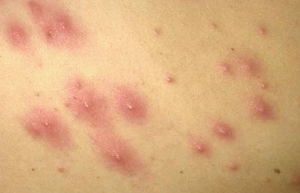
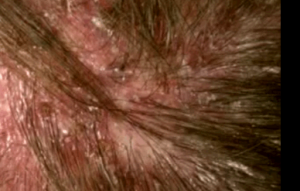


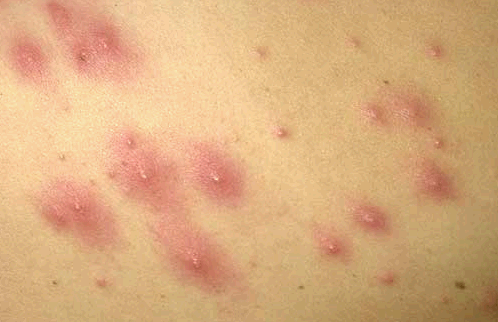
过年好! 查询优惠卷 进入腊月,集市上又红火热闹起来,年味也越来 专享优惠券 越浓了 小时候,觉得一年时间过得好慢。可能是因为过年可以吃到自己喜欢的糖果、美食,穿上新做的衣服,攒到长辈送给的压岁钱,可以燃放 淘宝优惠卷 烟花爆竹 ,但我觉得最主要的原因,还是希望自己能快点长大,早点进入成年人的世界。而今长大成人了,却再也无法感觉到憧憬中的那般美好,焦虑,担忧,压力 ,总觉得时间过得太快,还有很多事情没有完成。可叹,前辈们总是提前承受着晚辈们浑然不知的事情,此时此刻,站在光阴似箭的时间面前,我们依然是恍惚、盲从 ,不知不觉间,一年又即将过去。从王安石的诗词《元日》: 爆竹声中一岁除,春风送暖入屠苏。千门万户日,总把新桃换旧符 。注释:爆
他说我是长公主不久前在网上邂逅了他,他说他可以成为我的垃圾桶,我有什么话都可以往他这只垃圾桶里倒。我不以为 XC6SLX150T-3FG900I 然,那我不成大傻瓜了吗,我心里的话多着呢,岂是随随便便就可以对别人说起的。再说我有多年的闺蜜 XC6SLX100T-3FGG676C 、好友、同学、姐妹,彼此可谓很了解,就是这样,我都不会把心里的各种小心思和盘托出,而是有选择地该对谁说不该对谁说,在表达情绪的问题上,我谨慎着呢。与他有一搭无一搭闲侃了两回,他居然说你是个聊天对手,与你有的可聊,你骨子里的傲气,不一般,你 XC6SLX150T-2FG900I 就是个长公主。什么,什么长公主,我就是一个家庭妇女。你可不是家庭妇女,一听你说话就知道你从来都是导师居高临下,骨子里的长公主气势,当然你自已是不觉得的。这年头谁还没
面对欺骗的存在,我应该害怕吗?人这一辈子,要遇得不少骗子,有感情的骗子,有骗钱骗物的骗子,还有精 XC6SLX100T-2FG676C 神力的骗子。我是真的很害怕骗子的,宁愿不接触任何人,也不愿意被骗。如此极端,真的好吗?虽然不想承认,但是现实就是这 XC6SLX150-N3FGG900I 样,骗子真多。也许别人无心骗你,也许别人只是不想在弱鸡身上花费力气。也许,骗子带来的回报巨大,让骗子愿意投入。其实,还有一层原因,就是骗子的逻辑实在太简单了。撒谎这件事,不需要教,几乎看一遍就会。特别是在自己被骗过之后,印象深 XC6SLX150T-2FGG484C 刻久久不能忘怀。就是这样的刻骨铭心,让被骗的,即将成为骗子的人爱上了这种感觉。谁不想用最简单的方法,最有效地获得利益呢。而这种拙略的欺骗,往往效果不错,因为受骗的人